 In today's fast-paced world, many individuals are seeking holistic approaches to healthcare that address not only symptoms but also the underlying causes of illness and promote overall well-being. Osteopathy is
Read more
In today's fast-paced world, many individuals are seeking holistic approaches to healthcare that address not only symptoms but also the underlying causes of illness and promote overall well-being. Osteopathy is
Read more
-
Holistic Health Care: Integrating Osteopathy into Your Wellness Routine
posted: Apr. 18, 2024.
 In today's fast-paced world, many individuals are seeking holistic approaches to healthcare that address not only symptoms but also the underlying causes of illness and promote overall well-being. Osteopathy is
Read more
In today's fast-paced world, many individuals are seeking holistic approaches to healthcare that address not only symptoms but also the underlying causes of illness and promote overall well-being. Osteopathy is
Read more
-
Geriatric Osteopathy: Improving Mobility and Quality of Life in Older Adults
posted: Apr. 03, 2024.
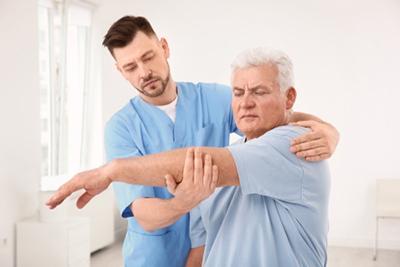 As we age, maintaining mobility and quality of life becomes increasingly important for overall well-being. Geriatric osteopathy, a specialized branch of osteopathic medicine, offers tailored treatments aimed at addressing the
Read more
As we age, maintaining mobility and quality of life becomes increasingly important for overall well-being. Geriatric osteopathy, a specialized branch of osteopathic medicine, offers tailored treatments aimed at addressing the
Read more
-
Sports Injuries and Osteopathy: Rehabilitation and Performance Enhancement
posted: Mar. 21, 2024.
 Sports are great for keeping you in shape. Unfortunately, playing a sport can also lead to experiencing a sports injury, especially if you are not in good physical condition, or
Read more
Sports are great for keeping you in shape. Unfortunately, playing a sport can also lead to experiencing a sports injury, especially if you are not in good physical condition, or
Read more
-
What Is Osteopathic Medicine
posted: Mar. 12, 2024.
 Osteopathic medicine is all about prevention to keep you well, so you enjoy a long, active life. When you are ill, osteopathic medicine uses all of the latest techniques and
Read more
Osteopathic medicine is all about prevention to keep you well, so you enjoy a long, active life. When you are ill, osteopathic medicine uses all of the latest techniques and
Read more
-
What To Know About Chronic Disease
posted: Mar. 07, 2024.
 Chronic diseases can be debilitating, affecting your mobility and quality of life. Chronic diseases can also lead to mental health issues, like depression and anxiety. If you are trying to
Read more
Chronic diseases can be debilitating, affecting your mobility and quality of life. Chronic diseases can also lead to mental health issues, like depression and anxiety. If you are trying to
Read more
-
The Importance of Preventive Healthcare
posted: Mar. 05, 2024.
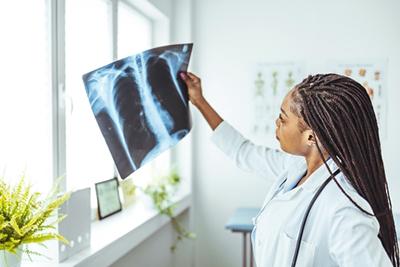 Prevention is the key to avoiding illness and disease. Preventive healthcare is especially important to avoid many chronic diseases, which can develop over time. Your osteopathic doctor is all about
Read more
Prevention is the key to avoiding illness and disease. Preventive healthcare is especially important to avoid many chronic diseases, which can develop over time. Your osteopathic doctor is all about
Read more
-
Osteopathy and Sports Injuries: Rehabilitation and Performance Enhancement
posted: Feb. 09, 2024.
 Playing sports is great exercise. Unfortunately, playing sports also puts you at risk of injury, especially if you are a weekend warrior, or are just getting into shape. If you
Read more
Playing sports is great exercise. Unfortunately, playing sports also puts you at risk of injury, especially if you are a weekend warrior, or are just getting into shape. If you
Read more
-
Osteopathic Medicine and Chronic Conditions: Managing Long-Term Health Issues
posted: Feb. 07, 2024.
 When you’re dealing with a chronic condition, it can impact how you feel every day. You might deal with constant pain and not be able to find the relief that
Read more
When you’re dealing with a chronic condition, it can impact how you feel every day. You might deal with constant pain and not be able to find the relief that
Read more
-
Osteopathy and Sports Medicine: Enhancing Performance and Preventing Injuries
posted: Jan. 11, 2024.
 If you’re an athlete, you need your body to be working at its highest potential. This means ensuring that any issues are dealt with effectively and that the root cause
Read more
If you’re an athlete, you need your body to be working at its highest potential. This means ensuring that any issues are dealt with effectively and that the root cause
Read more
-
The Osteopath's Role in Chronic Disease Management
posted: Dec. 26, 2023.
 Chronic diseases are prolonged health conditions persisting over months to years, often manageable but not easily curable. They encompass a wide range, like heart disease, diabetes, arthritis, and asthma. Common
Read more
Chronic diseases are prolonged health conditions persisting over months to years, often manageable but not easily curable. They encompass a wide range, like heart disease, diabetes, arthritis, and asthma. Common
Read more
-
Understanding the Role of Osteopathic Physicians in Primary Care
posted: Dec. 07, 2023.
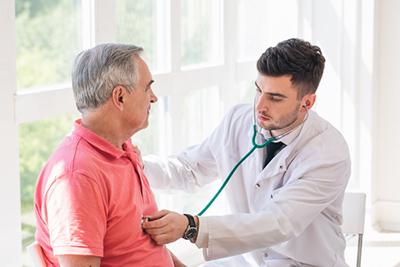 Conventional medicine relies on reactive treatments, which are treatments delivered after you are sick or injured. Osteopathic medicine is different. An osteopathic physician focuses on prevention, providing care to keep
Read more
Conventional medicine relies on reactive treatments, which are treatments delivered after you are sick or injured. Osteopathic medicine is different. An osteopathic physician focuses on prevention, providing care to keep
Read more
-
Treating Your Shoulder Pain
posted: Nov. 27, 2023.
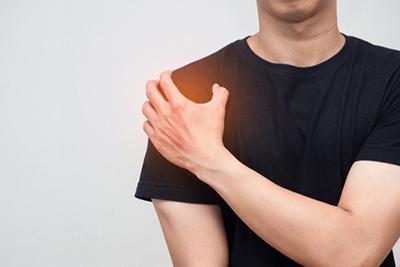 Shoulder pain can interfere with your life in various ways. If you’re dealing with constant shoulder pain, it can be hard to function properly or feel comfortable doing your daily
Read more
Shoulder pain can interfere with your life in various ways. If you’re dealing with constant shoulder pain, it can be hard to function properly or feel comfortable doing your daily
Read more
-
What Exactly Is Osteopathic Medicine?
posted: Nov. 09, 2023.
 There are several different fields of medicine that are focused on caring for different areas of your life. One that you may not know much about is osteopathic medicine. Osteopathic
Read more
There are several different fields of medicine that are focused on caring for different areas of your life. One that you may not know much about is osteopathic medicine. Osteopathic
Read more
-
Holistic Approaches to Health: Osteopathy and Wellness
posted: Oct. 27, 2023.
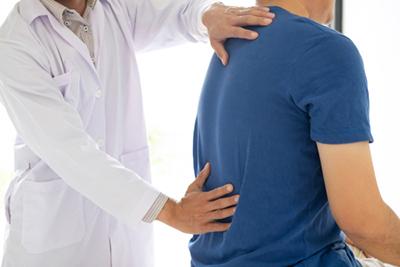 Instead of visiting a doctor and having them treat your symptoms, you may want to consider an osteopathic approach. With osteopathy, your doctor looks at your body as a whole
Read more
Instead of visiting a doctor and having them treat your symptoms, you may want to consider an osteopathic approach. With osteopathy, your doctor looks at your body as a whole
Read more
-
Preventive Care Is the Key to Health
posted: Sep. 18, 2023.
 Osteopathic medicine is all about looking at your body as a whole. You aren’t just a series of symptoms; everything is related and there are certain issues that may appear
Read more
Osteopathic medicine is all about looking at your body as a whole. You aren’t just a series of symptoms; everything is related and there are certain issues that may appear
Read more
-
Importance of Osteopathic Care
posted: Sep. 05, 2023.
 Osteopathic care is a holistic approach to medicine that focuses on your body's interconnectedness and ability to heal itself. It combines traditional medical practices with manual manipulation of muscles, bones,
Read more
Osteopathic care is a holistic approach to medicine that focuses on your body's interconnectedness and ability to heal itself. It combines traditional medical practices with manual manipulation of muscles, bones,
Read more
This website includes materials that are protected by copyright, or other proprietary rights. Transmission or reproduction of protected items beyond that allowed by fair use, as defined in the copyright laws, requires the written permission of the copyright owners.
